CASE STUDY • HEALTHCARE SPECIALIST PROVIDER GROUP
By Bill Frack, Chief Development Officer
Best-of-breed Unbundling Saves 10%
Vendor Stack Optimization Yields $1M Boost to Bottom Line
Hiring Wellnecity
In March 2021, the client was like many other growing specialty groups – focused on building a brand in its geographic footprint, integrating practice operations, and normalizing benefits. The group was also looking to leverage its platform to improve quality and move towards value-based contracting.
For the new CEO brought on board to lead this evolution, managing for quality needed to apply to the 2,400 members on the company’s health plan as well. Having led population management efforts for a large hospital system, the new CEO was confident he could meet those objectives with Wellnecity’s enablement.
While the ultimate focus would be on improving quality, the current configuration – a full-service, large carrier ASO (Administrative Services Only) and limited HR resources managing through Covid – would constrain options.
Phase 1
Getting Alignment and Setting the Stage
Wellnecity’s initial performance assessment highlighted several opportunities for (1) improved quality, e.g., better provider selection and polychronic member support, and (2) cost management, e.g., specialty medicines. However, the renewal process was well underway, and the carrier had placed several penalties in the contract if vendors such as the pharmacy benefit manager (PBM) were switched.
While Wellnecity demonstrated that the economic impact net of these penalties was compelling, the momentum for continuity was too strong. Therefore, near-term focus shifted to setting the stage for proactive management, i.e., getting alignment around and educating on best-of-breed solutions and tightening oversight of vendors.
Wellnecity helped the broker team explain the benefits of best-of-breed solutions, which enabled the client to get started with an independent stop-loss carrier, saving money on their renewal. Wellnecity also worked with the existing pharmacy consultant to highlight the inability under current PBM configuration to implement any clinical management programs to reduce accelerating pharmacy costs.
As further preparation for improved services, Wellnecity assessed the efficacy of carrier care navigation services. With no additional client team effort, Wellnecity implemented its suite of financial controls and vendor performance oversight tools. Savings were recognized from several eligibility reconciliations, improving Medicare education, and claims accuracy reviews.
Phase 2
Launching and Operationalizing High Value Programs
With renewal and open enrollment completed, in early 2022, Wellnecity put forward three programs which could be implemented during
the year (and would be consistent with anticipated 2023 plan moves). Those programs included:
- A national Center of Excellence solution (excluding the client’s own provider specialty, of course)
- A support program for the polychronic population (6% of members representing 30% of health plan spend), and
- A clinical program for improved specialty medicine sourcing
Given the potential positive impact on quality and cost, the physician-comprised board approved moving forward.
The specialty medicine sourcing opportunity was deferred to the end of the year to coincide with migration to flexible pharmacy benefit management. Wellnecity and the broker team selected a preferred care navigation partner. Care navigation has already been activated and Wellnecity is currently working on the integration between the care navigation partner and the Center of Excellence solution.
Phase 3
Establishing Best-of-Breed Pharmacy
Leveraging the previously provided research and insight provided by Wellnecity, the broker team and pharmacy consultant set out to conduct a full market evaluation of the client’s pharmacy benefit manager and owned-and-operated carrier administrator in order to enable decision-making around potential migration.
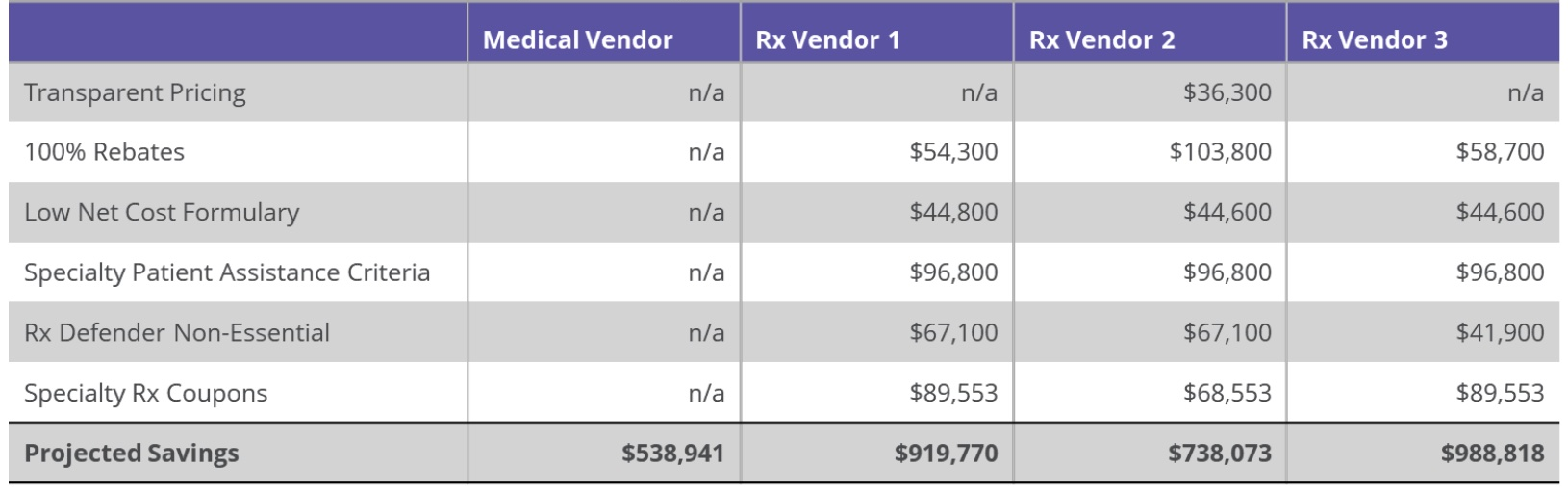
Wellnecity supported the process with additional insight and analyses and recommended transparent PBM options that were proven performers in Wellnecity’s client portfolio. With contracts recently signed, the client is expected to save almost $1M on their pharmacy spend – a 35% reduction in total pharmacy cost.

Critical to these savings was the ability to integrate best practice clinical programs to better manage quality and cost effectiveness. Wellnecity has begun the integration process with the new vendor towards the objective of optimizing implementation, avoiding early transition surprises, maximizing clinical program effectiveness, and managing multi-year trend by linking historical PBM data.
Exhibit: Year 1 Contract and Enhancement Projected Savings