CASE STUDY • NATIONAL HOME HEALTH OPERATOR
By Leo Raudaschl, VP of Finance
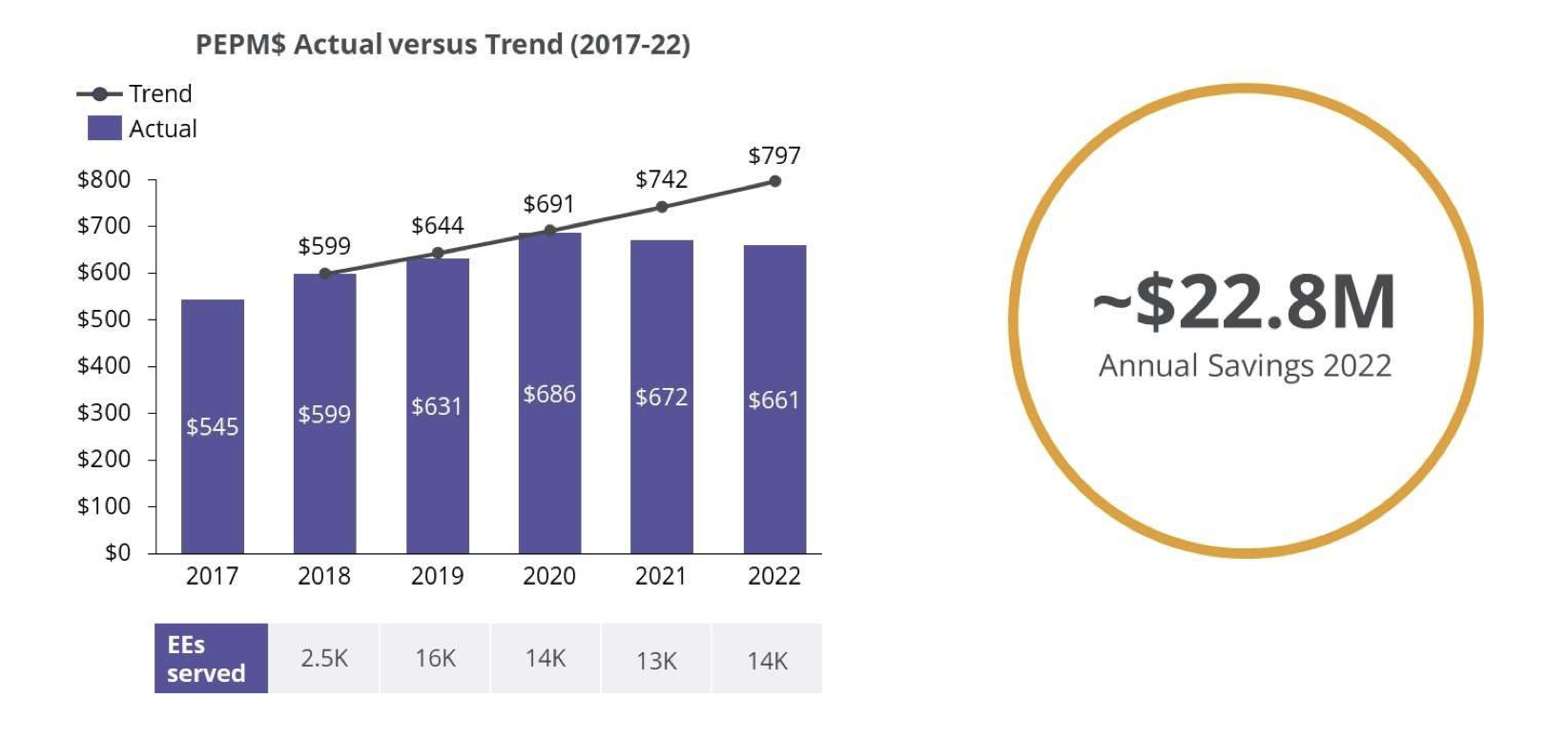
Maintaining 2% PEPM Trend Growth
Saves $20M+ Annually
Hiring Wellnecity
This client was Wellnecity’s first client – we were hired based on the promise of using the actual health plan data instead of subjective industry benchmarks as the basis for improved health plan management. As the CEO at the time said, “I have been looking for this type of help for years and it hasn’t existed. You’re hired.”
And so, an extraordinary journey began, managing a health plan through mergers and acquisitions and divestitures – with limited growth in PEPY, saving the company $20M on a 2022 run rate basis, and offering market competitive benefits.
Phase 1
Introducing Operational Oversight

In the first generation of Wellnecity, value was driven by proactive data management. Rather than relying on prepackaged reporting, the client and Wellnecity used the data to actively manage the plan—strengthening health plan oversight and vendor performance management, securing meaningful guarantees at renewal, and “tightening the ship” by identifying and resolving contract, claim, and enrollment errors.
As the organization evolved—following a merger and multiple plan changes, including a new PBM and network—the need for disciplined oversight became clear.
In one instance, just four months into deployment, the new PBM was already substantially over budget. Wellnecity identified the issue in month two—before the broker/consultant team had received top-line data—then isolated the drivers of variance and worked with the client, broker, and PBM to correct course and return to the expected run rate.
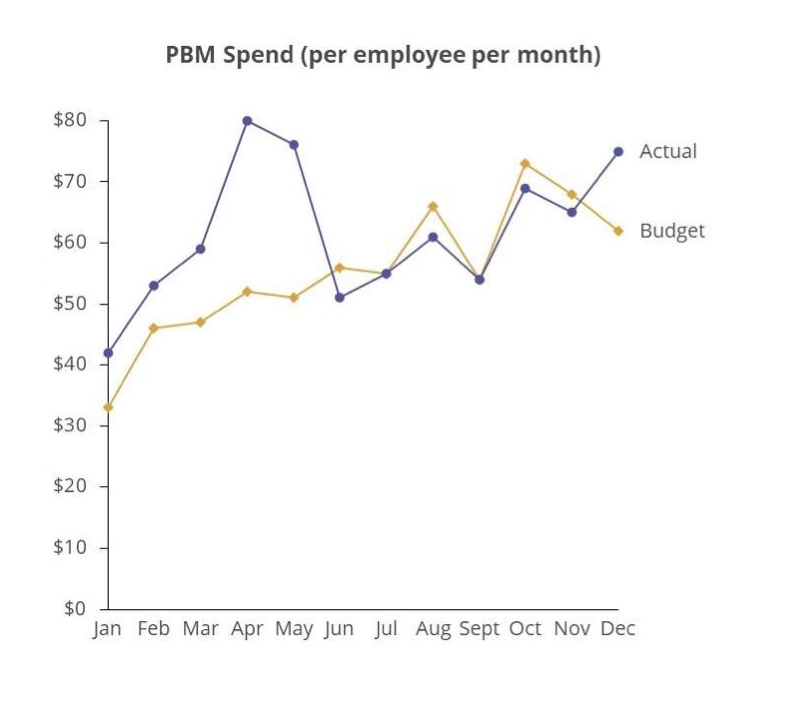
In a second instance, a negotiated reduction in the carrier administration fee was not being fully implemented. Wellnecity identified the gap and secured a retroactive recovery to the beginning of the year, resulting in $500,000 in savings.
With healthcare costs often representing a company’s second-largest expense, the impact of disciplined management extends beyond the health plan itself. In this case, savings helped offset broader operating pressures—enabling the client to preserve and distribute bonuses in one year and consistently minimize premium increases over time.
Phase 2
Building a Better Vendor Stack
As the plan grew in scale and sophistication, so did efforts to manage performance with vendor augmentations targeting improved care management, e.g., Centers of Excellence, Care Navigation, Diabetes Management, and Musculoskeletal (MSK) Management. Wellnecity’s role was to evaluate expected performance prior to vendor selection, ensure rapid and effective deployment, and optimize performance over time.
A key success was increasing utilization of the Center of Excellence from 15% to 45% of eligible cases—improving care by reducing unnecessary procedures and complication rates. Wellnecity developed a claims-based targeting algorithm that enabled care navigators to proactively engage members when the benefit was most relevant.
The impact was significant enough that the Center of Excellence vendor engaged Wellnecity to support broader engagement efforts. To enable this, Wellnecity aligned vendor processes, facilitated dynamic data exchange, and drove ongoing performance improvement.
For example, the MSK management program depends on early identification of care needs to guide members to high-quality, cost-effective providers. Wellnecity established new data feeds and enhanced pre-certification with key coding categories to support proactive outreach—resulting in strong early engagement.
Across point solutions, Wellnecity continues to optimize performance—driving conversion rates well above industry norms and measuring impact through real population outcomes and cost savings, rather than retrospective actuarial analysis.
Phase 3
Navigating Through Covid
As with most organizations, operating management took on a new level of complexity in Spring 2020—especially for healthcare-focused populations.
Early on, Wellnecity used data to provide a clear view of the actual Covid impact within the population—when reliable external data was limited. This included insight into health plan cost implications and projected future costs tied to severe cases and ongoing care.
As the situation evolved, focus shifted to critical operating decisions around workforce deployment. Wellnecity developed models to track vaccination rates and infection severity, helping guide informed back-to-work policies during an uncertain and rapidly changing environment.
As conditions stabilized, Wellnecity provided clear visibility into Covid-related utilization and vaccination trends, enabling leadership to confidently scale down Covid-specific support.
Finally, Wellnecity enabled the client to secure pre-allocated government financial support by isolating the Covid-related impact on the health plan and providing the required documentation.