CASE STUDY • REGIONAL AUTOMOTIVE DEALERSHIP
By Tony Giberti, Chief Operating Officer
Client Reversed 30% Year-Over-Year Health Plan Spend Increase
Phase 1
Measuring Plan Performance
Hiring Wellnecity
A sizeable regional automotive dealership engaged Wellnecity to integrate, standardize, and securely store its health plan data.
At the time, the client was facing escalating costs, an underperforming plan, and no visibility into the underlying drivers.
Wellnecity was engaged to measure performance, identify cost drivers, and recommend defensible data-driven strategies to improve benefit quality and end unsustainable year-over-year spend increases.
The client and their nationally recognized benefits consultant had previously discussed the need for change but lacked the data to support a meaningful overhaul.
Wellnecity conducted an independent performance assessment across medical, pharmacy, and eligibility data — both historical and current — verifying the 30% year-over-year cost increase and identifying the underlying cost drivers.
For the first time, leadership had objective, defensible data to support plan-level decision making.
“Armed with Wellnecity’s insights, I was able to get our executive team to make decisions on annual benefits in 30 minutes that previously we found impossible to reach consensus on.”
Phase 2
Immediate Improvement with Opportunity Pipeline
Wellnecity translated the performance assessment into a prioritized opportunity pipeline focused on immediate, defensible cost control and improved benefit quality.
The analysis identified targeted interventions across high-cost claimants, emergency department utilization, and specialty pharmacy spend — each supported by objective benchmark comparisons and actionable implementation strategies.
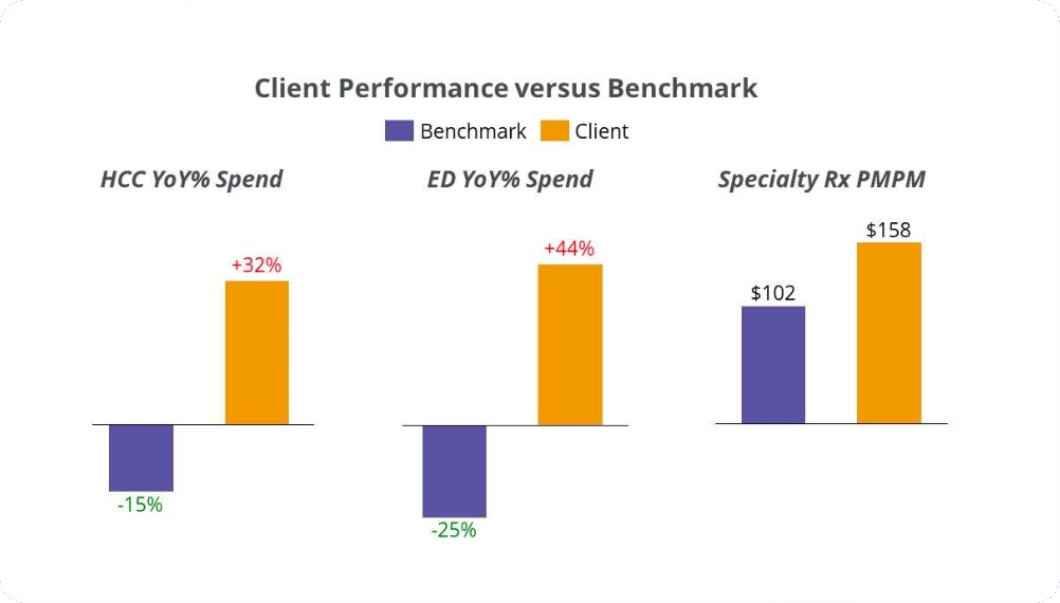
While the client focused on overall costs, they lacked visibility into the specific factors driving the increases. Wellnecity’s proprietary Performance Assessment revealed three primary drivers: high-cost claimants, elevated ED usage, and specialty pharmacy spend — each notably above benchmarks for like-size companies over the same period.
High-Cost Claimants
Wellnecity proposed a Centers of Excellence program targeting $400K–$500K in annual savings, plus polychronic management to improve adherence and reduce waste across chronic conditions.
Emergency Department
A Nurse Practitioner line reduced ER utilization through targeted outreach, generating $140K in annual savings. An HR education campaign also helped redirect non-emergent care to urgent care settings.
Specialty Pharmacy
Wellnecity recommended targeted international sourcing for specialty drugs, which improved utilization, and generated $200K in verifiable post-rebate savings within months through active management and member incentives.
Phase 2 Key Outcomes

Phase 3
Vendor Optimization & Evergreen Opportunity
Initial Prioritized Opportunity Pipeline
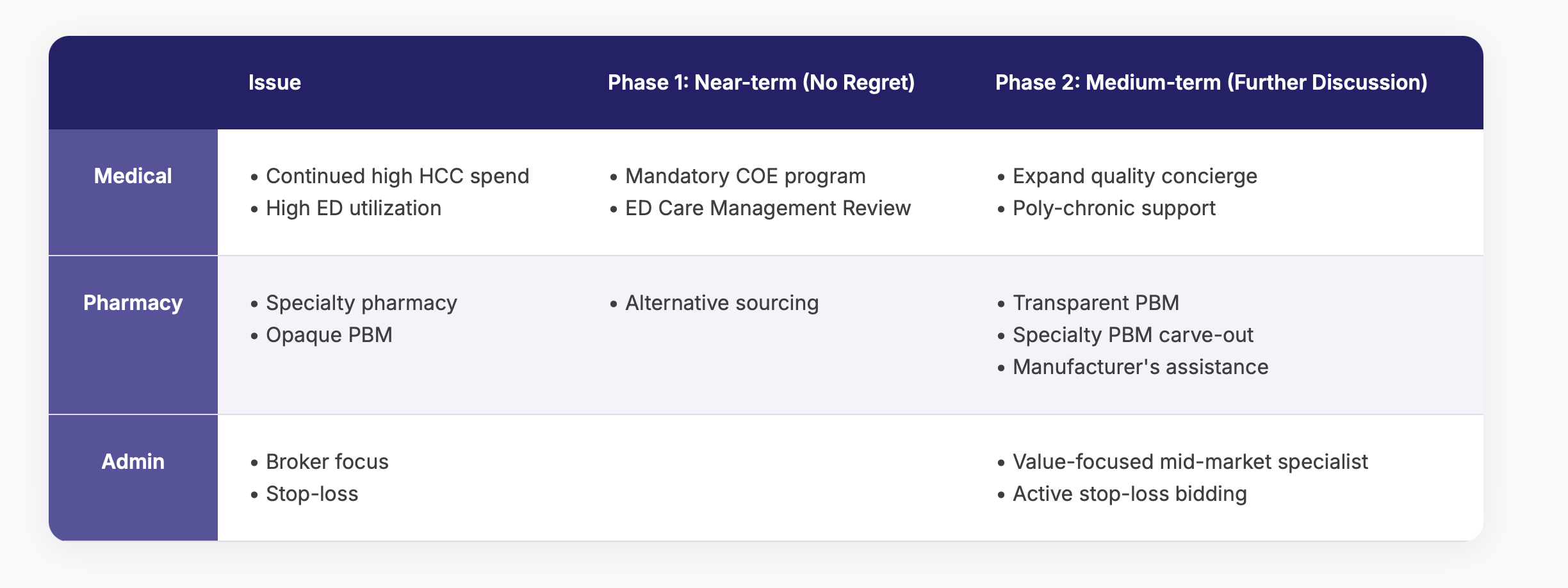
The client appreciated Wellnecity’s data-driven, independent perspective. As a result of our trusted working relationship, the CHRO reached out to improve its core vendor configuration — ultimately engaging a new PBM and switching to a more effective carrier. This move was not initiated by the broker.
Under the new carrier, Wellnecity realized significant one-time stop-loss reconciliation value in addition to ongoing performance savings through a transparent PBM and new TPA.
The team continued to drive value, turning alternative Rx sourcing into an evergreen value lever, making the client the only employer in their national Rx coalition outperforming benchmarks.
Wellnecity enabled vendors to perform better by providing them with crucial information they did not have. For example, targeted claims and eligibility data supported outreach for mental health, hospital discharge, and screenings, improving efficiency and effectiveness. One nurse shared, “I want Wellnecity working for all my clients.”
