CASE STUDY • REGIONAL NURSING HOME OPERATOR
By Bill Frack, Chief Development Officer
Vendor Stack Reconfiguration Saves
25% Per Employee
Hiring Wellnecity
A regional senior care and nursing home company with 800 employees engaged Wellnecity to control rising healthcare costs. In a low-margin environment, they were evaluating a shift from a bundled Aetna solution to a best-of-breed model with point solutions.
The goal was clear: no increase in cost per employee—and no added cost to employees. Wellnecity deployed in mid-May to drive immediate impact.
The engagement focused on two challenges: vendor overload and limited visibility. Wellnecity assessed performance and identified strategies to improve outcomes while controlling costs.
Phase 1
Carving Out

Wellnecity was engaged at the beginning of the annual renewal process. While self-funded, the client was receiving bundled benefits from a national health insurance payer. They were also exploring reference-based pricing (RBP) as an alternative to reduce costs. Wellnecity’s experience with RBP vendors from other clients, coupled with Wellnecity’s ability to support the implementation process gave the client the confidence to proceed with the switch. While the savings from RBP would be impressive (13+% of medical), there was more opportunity to optimize the plan with a total “carve-out”, i.e., unbundling of benefits.
As expected, the current health insurance provider presented an aggressive counter proposal. While having a national brand on the benefits card was attractive, the total cost improvement could not be overcome. The client decided to proceed with the carve-out as planned to gain control over their health plan spend.
The client, with their benefit advisors, supported by Wellnecity’s insights and analytics, contracted with a new transparent Pharmacy Benefits Manager (PBM) with active clinical programs, and shopped extensively to obtain an excellent stop-loss policy. Net overall savings were 25% per employee per month (PEPM), saving the client well over $1M.
Phase 2
Operational Support
The time to evaluate the counter proposal compressed the schedule to complete the transfer of benefits. This required rapid action by the client and the plan administrator. To facilitate a timely transfer, Wellnecity leveraged its data management capabilities, extracting information from the benefits administration system, and transferred it to the third-party administrator (TPA) in the requisite format resulting in the seamless continuation of benefits. Wellnecity then managed the eligibility interface for several weeks until the TPA and RBP vendor were fully operational.
In addition, Wellnecity established a new approach to RBP negotiations, verified diabetic members’ adherence to insulin regimens while identifying lower cost Rx solutions, optimized plan enrollment, and renegotiated more favorable contract terms during the renewal process.
RBP Negotiations
The RBP model was stabilized within 6 months during the start Covid-19 pandemic; however, the client was not happy when some providers began to challenge the negotiated rates. In these instances, new negotiations were triggered causing friction for both HR and the impacted plan members. Wellnecity intervened and worked with the client and RBP provider to set a floor for acceptable negotiations and outcomes. This improved the member experience and significantly reduced the administrative burden of reconciling these issues.
Medication Adherence and Improved Rx Sourcing
In addition, the client was concerned that changes to the high-deductible plan were impacting diabetic members’ adherence to their insulin regimen. Through targeted analysis, Wellnecity was able to show that the January deductible reset was not causing members to miss their insulin. Wellnecity also advised that improving the implementation of the international Rx sourcing programs could reduce insulin costs for members.
Plan Optimization
In parallel, Wellnecity scrutinized plan participation, focusing on Dependent Eligibility and Medicare Eligibility. In both instances, Wellnecity managed a customized process to identify and remove ineligible dependents and educate members 65 and older on more attractive Medicare Advantage options. Each effort reduced plan spend by approximately $80,000, and ensured ERISA compliance, with negligible involvement from HR.
Contract Reconciliation
Wellnecity also identified a $50,000 per year payment to a pharmacy vendor not delivering value due to the restrictive contract of the previous plan provider. The contract was renegotiated through the renewal process, and this spend was eliminated.
Phase 3
Improving Care
Wellnecity also continues to focus on the quality of care. In response to an increasing number of cancer cases, a center of excellence program is being implemented. This will give plan members access to nationally ranked providers when cancer care in the community is challenged to keep up with the rapid advances in treatments and emerging technologies.
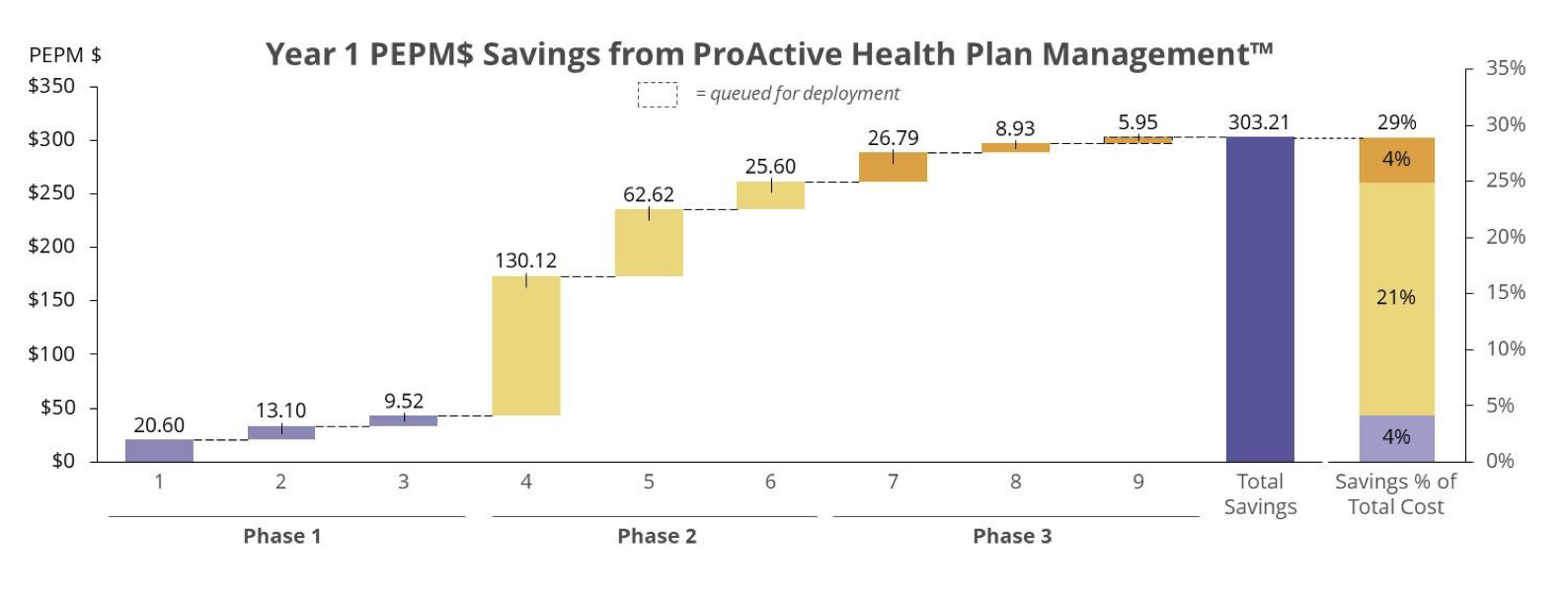
Overall, the client has saved more than 6 times the fees paid to Wellnecity (over and above the switch to RBP), representing a PEPM plan savings approaching 30 percent. Because Wellnecity is integrating data from the previous plan with the vendor data from the new RBP provider, the client can confidently and continuously monitor and measure the impact of their health plan.
The journey to sustain improvements in cost and quality continues. Wellnecity enabled this senior care and nursing home company to proceed confidently despite the inability to expand HR during the Covid-19 pandemic – and benefit from outcomes that turned out to be much greater than the original value proposition.