By Bill Frack, Chief Product Officer and Mike Maley, Head of Product
Situation
The journey to treat cancer is arduous, complicated and expensive. Cancer care is the leading category of cost for high-cost claimants in many employers’ health plans. Effective cancer care is a function of three key variables:
- Timely discovery – early stage cancers are easier to address
- Right care team – deploying the right resources leads to better outcomes at lower cost
- Right support – providing additional member support helps the patient and their family through the process
In this three-part series, we will address each variable in sequence, starting here with timely discovery. It is well understood that early detection leads to better outcomes, higher survival rates, and lower cost of treatment.
Complication
The challenge for employers is to maximize compliance with well-established screening guidelines – current compliance levels are low. For each type of cancer, e.g., breast, which has an accepted screening guideline, there are broadly accepted eligibility criteria based on age and other risk factors, and testing intervals. Earlier diagnosis leads to better outcomes so the merit for compliance seems obvious. Yet, often less than 50% of people that should be screened, actually are. In addition to general awareness of the need for screening and qualifying criteria, several compounding issues like perceived cost and convenience contribute to poor screening rates and, as a result, later detection requiring more invasive treatment.
Sadly, many employers believe they are doing the best they can. Why? Because brokers and carriers normally benchmark employers against their peers, rather than a reasonable best practice. Case in point: the national average for PPO plans for colon cancer screening is 35%. The best practice observed is actually approximately 75%. That’s a lot of people who could be screened and have their cancer detected while the disease is easier to treat. There is substantial difference in the outcomes treating stage 2 colon cancer and treating stage 4 colon cancer, as the later stage cancer often can require a combination of multiple surgeries, high-cost medications, chemotherapy, radiation therapy, as well as more complexities, complications, and higher risk of recurrence than a cancer caught at an earlier stage. In fact, given average screening rates at a typical employer – just over 3 people per 1000 have diagnosable colon cancer that could be being treated today.
Solution
The solution is straightforward: 1) Understand your screening gap and 2) Close the gap.
To understand your gap, compare your performance to best practices, not your peers. Ask your advisor and carrier for your numbers if you don’t already have them (if they can’t provide the information, you have a more fundamental problem). Compare your numbers to the “achievable best practice” in the example below to define your mission. Which cancers do you want to focus on? Where is the biggest gap? What improvement will yield the most benefit?
To close the gap, you need to better understand who in your population is not compliant with screening guidelines. Wellnecity creates a profile of the unscreened population and, for employers interested in direct outreach or targeted marketing, a target list. If you don’t have the detail, you can still improve messaging and incentives, but you won’t be as on target. In addition to better informing your associates, consider solutions that facilitate compliance such as mobile testing units. If your employees are co-located, a full event can be created.
Finally, if you really want to get proactive, keep an eye on Grail. This company has developed a multi-cancer blood test called the Galleri test, which covers many previously unscreenable cancers. The “liquid biopsy“ solution space is expected to develop rapidly.
Above all, get informed and get active. Lives are at stake.
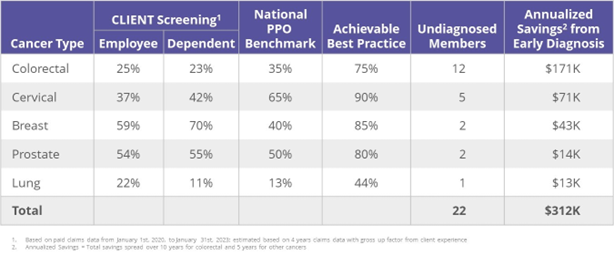
Wellnecity Example
The following exhibit of screening rates is from a Wellnecity client in the physician services space. The table demonstrates the gap in current performance, the lives impacted, and the projected cost impact due to potential later-stage discovery. The annualized savings are based on avoided direct treatment cost and do not include the added non-trivial burden on patient and family, or lost work.